|
Assessing Trauma
in Sierra Leone
Psychosocial Questionnaire: Freetown Survey Outcomes by Kaz de Jong, Maureen Mulham, and Saskia van der Kam January 11, 2000 This report is the product of close cooperation and hard work by a multinational team motivated to bear witness to the anguish suffered by the Sierra Leone population. Warm thanks to MSF-Holland’s medical coordinator in Freetown, Maureen Mulham, for skillfully guiding the survey process. Lo van Beers was instrumental during the data entry process. Special thanks go to the group of Sierra Leonian interviewers and their respondents for the difficult and often painful work of asking and answering the survey questions. For reasons of security, the names of the interviewers/interviewees cannot be given. — Kaz de Jong, Mental Health Advisor, MSF-Holland (January 2000) I. Summary This report is based on a mental health survey of persons in Freetown, Sierra Leone in May 1999. Several months earlier the city saw fierce fighting that left more than 6000 people dead, an untold number injured and mutilated, and tens of thousands homeless. Many of those affected had gone through similar experiences before, and had fled to Freetown for its relative safety. The findings only touch on the sufferings of the country’s population. The civil war in Sierra Leone began in 1991 and no region has been spared. The residents of Freetown were not alone in their trauma: the country’s town and village dwellers too, have often been repeated victims of war, displaced time and again from their homes and subjected to terrible and long-lasting hardships. Although fighting in the country has largely ceased since the Lome Peace Accord of July 1999, the effects of that war will be with the population for a long time. As this survey makes clear, few escaped the mental trauma of the war zone that Freetown became for more than three weeks in January 1999. Doctors Without Borders found, among other things, that 99% of those surveyed suffered some degree of starvation, 90% witnessed people being wounded or killed, and at least 50% lost someone close to them. The intensity of the fighting is indicated by the numbers: 65% endured shelling, 62% the burning of their property, and 73% the destruction of their homes. Physical harm was also great: 7% had been amputated (typically a limb, hand, foot or ear), 16% had been tortured by a warring faction, 33% had been held hostage, and 39% had been maltreated in some way or another. The psychological impact of actually witnessing horrific events imposes a serious psychological stress. Deliberately or not, witnessing at least once events such as torture (54%), execution (41%), (attempted) amputations (32%), people being burnt in their houses (28%) and public rape (14%) often results in traumatic stress or even Post-Traumatic Stress Disorder (PTSD). Almost all respondents reported to have seen wounded people at least once (90%). Doctors Without Borders also found, through a technique called the Impact of Event Scale, that the population showed very high levels of traumatic stress. Traumatic stress associated with physical complaints like headaches (38%) and body pains (12%) is reported most frequently. The psychosocial and mental health consequences of war on civilians are all too often neglected. Even after hostilities cease, the war may continue in people’s minds for years, decades, perhaps even generations. To address only the material restoration and physical needs of the population denies the shattered emotional worlds, ignores the broken basic assumptions of trust and benevolence of human beings, and leaves unaddressed the shattered moral and spiritual consequences of war. After severe conflicts, people seek to forget or deny what happened to avoid painful memories of the past and to escape the sense of hopelessness, humiliation, and anger. But for the direct survivors of violence, acknowledgement of the suffering is a crucial element for making sense of and addressing traumatic experiences. To help a traumatized person there is a need to restore the bonds between the individual and their surrounding system of family, friends, community, and society. Overcoming the extreme stress and sometimes even severe mental health problems associated with mass traumatization such as occurred in Sierra Leone, tests the healing capacity of family and community. II. Background 1. Political Context In May 1997, military officers of the self-proclaimed Armed Forces Revolutionary Council (AFRC) overthrew the democratically elected government of President Ahmed Tejan Kabbah and formed a junta with the insurgent Revolutionary United Front (RUF). In February 1998, the West African peacekeeping force ECOMOG ousted the combined AFRC/RUF forces, whose remaining fighters fled to the countryside. President Kabbah was reinstated in office on March 10, 1998. In December 1998 the combined RUF/AFRC forces launched a massive offensive that brought the fighting into the capital, Freetown. The fighting in Freetown in January 1999 was an intense, violent repetition of the brutality that has become common in Sierra Leone. The rebel forces committed indiscriminate attacks – thousands of executions, abductions, and rapes – on the civilian population. Arson and looting were widespread. ECOMOG forces were implicated in the summary execution of hundreds of suspected RUF fighters. Altogether, some 6000 people died in Freetown over a three-week period and some 150,000 were displaced from their homes. When the rebels were forced to retreat, they cruelly amputated arms and legs and ears of civilians in their custody. On July 7, 1999 the various parties signed a Peace Accord in Lome. Since then, armed clashes have been sporadic, travel through most of the country is now possible, and Freetown is being rebuilt. But insecurity remains. The inadequately funded and ill-functioning Disarmament, Demobilisation, and Reintegration program has meant that too many armed soldiers and ex-soldiers roam the countryside. Too few of those abducted, including hundreds of children, have been allowed to return home. And continued lawlessness by the armed factions has sharply limited humanitarian access in those regions, particularly in the north and east, where assistance is most needed. 2. Medical Context Since 1994, Doctors Without Borders has provided medical and nutritional programs in Sierra Leone, including surgery, primary health care support, and water and sanitation. At the end of 1997, a psychosocial program was implemented around Magburaka in central Sierra Leone, but because of the security situation, the program was suspended. After the January 1999 events, Doctors Without Borders, through trained local counselors, started psychosocial care to amputees in the hospital in Freetown. Until recently, emergency medical programs have been dominated by a perspective emphasizing physical health and immediate relief. Behavioral, mental, and social problems were neglected. Since the genocide in Rwanda and the conflict in the Former Yugoslavia, it has become recognized that mental health and psychosocial programs can greatly contribute to the alleviation of the suffering of people in war and disaster-stricken areas (e.g. Ajdukovic, 1997). Focused primarily on the effects of post-traumatic stress, these programs have put the psychological consequences of massive man-made violence on individuals and populations on the agenda of the international community. Research has shown that nearly all war victims experience recurrent and intrusive recollections, dreams, and sudden feelings of reliving the event (e.g. Bramsen, 1996). These responses are combined with increased arousal, avoidance of stimuli associated with the trauma, and numbing. Through the oscillation between intrusions and avoidance, the psychological integration of the traumatic experience is realized, which has been made clear in cognitive processing models (e.g. Creamer, 1995). Physical symptoms such as headaches, stomach pains, and back pains are often part of this process. These physical symptoms frequently cause persons to seek medical attention. The occurrence of mass PTSD can have a debilitating effect on communities. Daily experience in the field demonstrates that traumatized people impede the restoration of ordinary life and jeopardize conflict resolution. Besides the mental and physical suffering that people experience, on a spiritual level their fundamental assumptions of control and certainty, as well as basic beliefs in the future and in the benevolence of other people, are also shattered--often beyond repair (Janoff-Bulman, 1992; Kleber & Brom, 1992). Research indicates that the duration and the frequency of traumatic experiences negatively influences physical, mental and spiritual coping mechanisms (e.g. Kleber & Brom, 1992). Post-Traumatic Stress Disorder (PTSD) is frequently used in connection with traumatic events. The concept is well fitted to describe the serious and prolonged disturbances of individuals confronted with major life events. The distinctive criteria of PTSD (Diagnostic and Statistical Manual of Mental Disorders, 4th ed. (DSM-IV); APA, 1994) are (1) an extreme stress, (2) intrusive and re-experiencing symptoms, (3) avoidance and numbing symptoms, (4) symptoms of hyperarousal, and (5) symptoms of criteria 2, 3, and 4 should be present at least one month. The concept is also included in the International Classification of Diseases (ICD-10) of the World Health Organization (1992). PTSD is strongly associated with dissociation and somatization (McFarlane, Atchinson, Rafalowicz & Papay, 1994; Van der Kolk et al., 1996). The concept of PTSD should be considered with care for several reasons. First, not all disorders after traumatic events can be described in terms of PTSD. It is not the one and only possible disorder after traumatic events, even according to the DSM system. Co-morbidity has been found to be more prominent in trauma patients than was originally assumed (Kleber, 1997). Second, whether western conceptual frameworks on psychological stress and mental disorders can be transferred to different areas of the world are practical as well as theoretical and ethical questions (Kleber, Figley & Gersons, 1995; Summerfield, 1996). Doctors Without Borders has been addressing the psychosocial problems of the survivors of violence in Sierra Leone before, during and after the January 1999 events. Doctors Without Borders is very concerned that neglect of the mental health and psychosocial problems of the large number of people who are suffering from prolonged traumatic experiences may cause serious problems for the future of Sierra Leone. Simply ending the war does not eliminate the problem. Doctors Without Borders decided to start a psychosocial program in Freetown. As part of its program, a population survey was conducted in Freetown to learn what people experienced, to what extent the events resulted in traumatic stress, and what other medical needs the inhabitants had. In the absence of other psychosocial surveys in emergency situations to serve as a model, the survey instruments were composed and partly designed by Doctors Without Borders. III. Methodology 1. Target Population & Sample The survey was conducted after receiving the permission of the appropriate authorities, during the first two weeks of May 1999, four months after the atrocities in Freetown. Because everyone in Freetown had been subjected to traumatic experiences, both Internally Displaced Persons (IDP’s) and residents were included in the sample. A two-stage cluster sampling method was used, a methodology based on vaccination surveys. The methodology is extensively described in the various handbooks of WHO. The sampling method entails a first phase where 30 clusters are chosen. In the second phase a pre-set number of individuals are chosen per cluster. The sampling technique itself ensures that every individual has an equal chance to be chosen. The result obtained through sampling techniques is an approximation of the real value in the entire population. The real population value is in a range around the value obtained by the sampling method. The narrower the range, the more precise is the estimation. The precision depends on the sample size and the inter-cluster variation and the intra-cluster variation of the specific survey. The precision of the results with this two-stage sampling technique is less than the precision one would get with a random sampling technique. The sample consisted of 30 clusters of 8 respondents, as the intra-cluster variation was thought to be reasonably small, since most traumatic events take place on a community level and not on an individual level. The sampling frame is based on the 1997 census of the Ministry of Health and UNICEF, which gives a population of 600,000. The rural part of the Western area (encompassing Freetown and its peninsula) was excluded because most of the area was not accessible during the survey for security reasons. The areas (clusters) were chosen with a chance proportional to the population size. The teams went to the center point of these areas; a pen was spun to determine the direction and every tenth house to the right was selected until the eight necessary for the cluster had been identified. The most senior member of the household present was interviewed. Any refusals were noted and the selection process continued to the next tenth house. There was a note made on each questionnaire of the displaced or resident status of the interviewee. Where the cluster was in a displaced camp one person from each section of the camp was interviewed, depending on the layout of the camp. Four survey teams were selected. Each team had to conduct eight interviews each day. All interviews were scheduled in the first two weeks. Eight interviews per day per team were the maximum due to the difficult nature of the information gathered. 2. Training The survey teams consisted of two trained local counselors who did the interviews and a support team of one expatriate staff member and a driver. The training consisted of the following elements: introduction to Doctors Without Borders, the nature and purpose of the survey, confidentiality of the data and information, survey technique, data registration and task division among crews. Some survey questions might have provoked strong emotions, so the counselors received special training on how to deal with them. They were also informed on referral possibilities for those in need of follow-up psychosocial support. Counselors practiced interviewing skills on each other. The items of the questionnaire were discussed in depth until a final interpretation was agreed on each question. A pilot study of eight interviews was carried out by the teams in the National Stadium IDP site, Kingtom area, Aberdeen Junction and Murray Town. After the pilot interviews, problems of interviewing, sampling and approaching people were discussed. Ambiguities in the questionnaire were addressed. The training (including the pilot study) lasted two days. 3. The Interview The counselors worked in pairs. After the counselors introduced themselves and Doctors Without Borders, the purpose of the survey was explained to the potential participant. In the introduction it was clearly stated that the participant would not receive any compensation, that the data were treated confidentially and that the interview would last for a maximum of 40 minutes. After the introduction the participant could decide whether to participate. The timing of the interviews was crucial, since people had to be at home and be available. It was important that the participants completed the survey. To avoid exceeding the interview time it was explained that direct and short answers were necessary. Extra discussions or conversations were avoided. However, the counselors were permitted to stop or interrupt the interview when they deemed the questions to be too emotionally upsetting for the participant. When the counselor believed that the participant needed follow-up support, referral to professional counselors was facilitated. All teams had a daily technical and emotional debriefing. Further emotional support for the counselors was provided through the Doctors Without Borders psychosocial peer support system for national staff, which was trained by the Doctors Without Borders Amsterdam Public Health Department and Psychosocial Care Unit. 4. The Psychosocial Questionnaire The structured interview was based on a questionnaire consisting of 35 questions with subdivisions. To control the time of the interview most questions offered a limited number of alternatives from which the participant could choose. Only two questions in the health section of the questionnaire were open ended. To limit the emotional burden the questions were put as factually and simply as possible. When unclear, a short explanation was allowed. Participants were not allowed to fill the questionnaire later nor were they permitted to study the questionnaire in advance. Interviewers had to respect confidentiality at all times. No trans-cultural tools to measure traumatic stress are available. To assess the level of trauma, three important indicators of traumatic stress were measured. The first indicator is the presence of a potential traumatic event. The second indicator is the impact of event scale, which expresses the extent of traumatic stress response. The third indicator appraises physical complaints, which likely are correlated to traumatic stress. When all three indicators of traumatic stress were positive, at least strong circumstantial evidence for the prevalence of traumatic stress was found. The psychosocial questionnaire was composed of four sections. The first section assessed the demographics and personal background of the participant. A second section appraised traumatic events such as exposure to violent situations, who was lost and the traumatic events witnessed. Both the number of traumatic experiences and their length are important risk factors in the development of PTSD (Kleber & Brom, 1992). The third section measured the impact of these events. To measure the prevalence of traumatic stress responses the Impact of Event Scale was used (Horowitz, Wilner & Alvarez, 1979). This psychometric instrument assesses two central dimensions of coping with drastic life events: intrusion and denial. It has been used worldwide and generally consistent structures have been found across samples and situations (Dyregrov, Kuterovac & Barath, 1996; Joseph, Williams, Yule & Walker, 1992; Robbins & Hunt, 1996; Schwarzwald, Solomon, Weisenberg & Mikulincer, 1987; Silver & Iacono, 1984; Zilberg, Weiss & Horowitz, 1982). Despite its wide use, interpretations of the outcomes should be done with appropriate care since the Impact of Event Scale is not validated either for Western Africa or for Sierra Leone. The final section of the questionnaire evaluated current physical health complaints and needs. PTSD is frequently associated with somatization. Physical symptoms like headaches, stomach problems, general body pain, dizziness or palpitations are often expressed by people suffering from traumatic stress. A high prevalence indicates a possible high level of traumatic stress or PTSD. Physicals are registered by means of open-ended questions. The access to health care and the perceived health levels were registered using the Lickerd scale. 5. Data registration The forms were registered anonymously. Data were entered in a spreadsheet in EXCEL, and data were analyzed by EXCEL and EPIINFO-6. IV. Results All four teams contributed equally to the survey (each 25%). The fixed number of interviews in each cluster (n=80) was extended in four clusters (Old Warf, Aberdeen, Approved School/Kuntoloh, National Workshop). The total number of respondents was 248 (n= 248), of which three respondents were excluded because they were younger than 15 years. 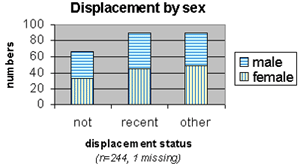
1. Demographics (First section) In total 91 (37%) respondents were recently displaced; only 66 (27%) were residents. The others (37%) could not be placed in one of these categories. A possible explanation is that many people had been displaced in earlier years. About half (52%) of the respondents were female (Confidence interval 95% level: 46.4 – 56.8). The age of the respondents varies from
15 up to 81 years with a majority of the respondents in the middle age
group of 35-44 years (29%).
2. Appraisal of traumatic experiences (Second section) Graph 3 shows what situations the respondents have faced. Incidents include: attack on village (84%), exposed to cross fire (84%), explosion of mines (28%), aerial bombing (83%), mortar fire (65%), burning of properties (62%) and destruction of houses (73%), indicating that large groups of the population of Freetown have been caught in direct war. In addition to the direct threats caused by the hostilities, the lack of food and other commodities forced people to take extra risks (74%). A smaller number of people (57%) had to walk long distances to find a safer place. The risk of abduction was clearly present since 43% of the respondents reported having been exposed to abductions. Generally half of the respondents indicate that the event had taken place more than three times. 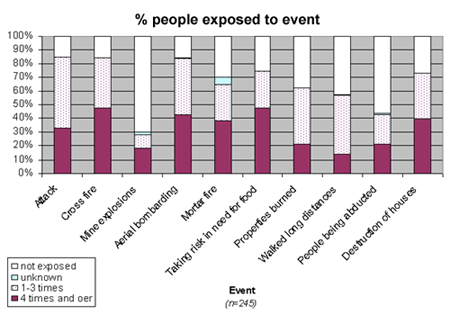
Coping with traumatic events is more difficult when people themselves experience immediate life-threatening circumstances (Kleber, Brom; 1992). Graph 4 shows what life-threatening traumatic experiences some of the respondents survived. The respondents were allowed to report on all items. The percentages are related to the number of people having experienced that event as a proportion of the total number of respondents. Several people suffered from multiple life-threatening experiences. 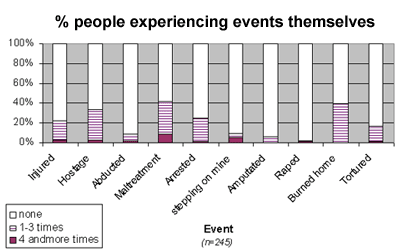
A high percentage of respondents directly experienced at least once an event threatening their physical integrity, either by maltreatment (39%) torture (16%) or amputations (7%). 40% of the respondents have seen their houses burned down; 33% were taken hostage. The percentage of people reporting abduction is, in contrast to the above, relatively low (7%). The relatively low report on rape (2%) should not be misinterpreted. Rape is, as in most other countries, a taboo topic. Rape victims usually do not report this crime to avoid serious repercussion from their family or to evade the stigma communities and society impose on these victims. The dire food situation is by far the highest life threatening experience, as it was reported by almost all the respondents (99%). 2.2 Loss and witnessing 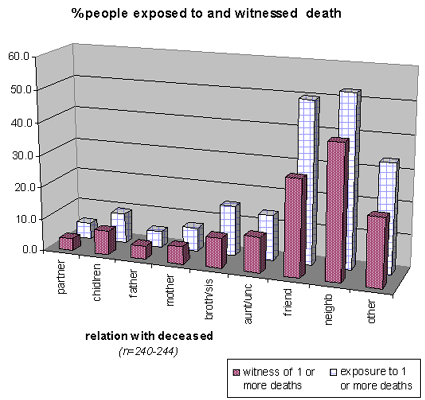
Conflict and violence are closely related to loss. Loss of loved ones and witnessing their violent death might be one of the most serious risk factors for PTSD. Graph 5 gives an overview of both. The percentage of people lost increases with the number available. The loss in the nuclear family (partner (5%), father (5%), mother (7%), child(ren) (9%) and siblings (16%)) is reported less then the loss of more "distant" family members (aunt, uncles (14%)). The percentages reported on death of neighbors (53%) and friends (50%), is clearly higher, since there are more of them. These data indicate that at least 50% of the respondents lost someone they knew very closely. Many respondents witnessed the death of a close person: 30% witnessed the death of a friend, 41% that of a neighbor. Additionally 7% witnessed the death of their child. 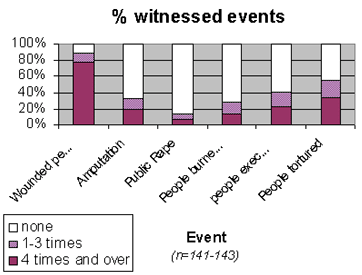
To create terror a perpetrator often demands others to witness the atrocities. The psychological impact of actually witnessing horrific events imposes a serious psychological stress. Deliberately or not, witnessing at least once events such as torture (54%), execution (41%), (attempted) amputations (32%), people being burnt in their houses (28%) and public rape (14%) often results in traumatic stress or even PTSD. Almost all respondents reported to have seen wounded people at least once (90%). Graph 6 gives an overview. 3. Impact of Event Scale (Third section) The inhabitants experienced horrific events. The third section measures the prevalence of traumatic stress responses through the Impact of Event Scale questionnaire (Horowitz, Wilier & Alvarez, 1979). The PTSD score as outcome of the Impact of Event Scale (I.E.S.), is constructed around two clusters of reactions. Intrusions such as flashbacks, nightmares and reliving the event are indicators of the preoccupation with the events that often characterize survivors of violence. Complaints like "I can't stop thinking about it" combined with the unpredictable occurrence of flashbacks often provoke feelings of having lost control or becoming crazy. To compensate for the agony of ongoing intrusions, survivors try to avoid situations, places, conversations or people that remind them of the events. The avoidance as well as the intrusions has a debilitating effect on the survivors' social life. Social withdrawal and a life obsessed by fear and avoidance may be the destiny of those that suffer from severe, chronic PTSD. 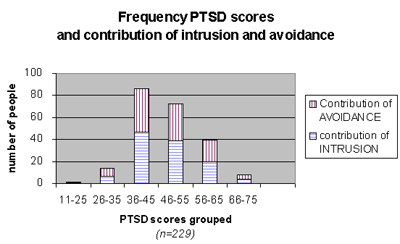
The overall PTSD scores registered on the I.E.S. are high. When the cut of scores (no problem: 0-10, at risk: 11-25, PTSD: 26-75) for Western Europe are applied, no one reports to having "no problem." Two people have scores indicating a risk for developing PTSD. All other respondents (99%) have scores on the I.E.S. that are associated with PTSD in a Western European setting. In the current survey most people (111, 27%) have scores between 36 and 45, which is similar to the number of people having scores between 46 and 55. Graph 7 shows the scores on the I.E.S. No significant differences were found between the contribution of intrusions and avoidance on the overall PTSD score. There were 16 respondents who were not able to give a clear answer on one of the questions composing the PTSD scale; these respondents are excluded from the total PTSD score. The average score on the PTSD scale was 47.6, with a confidence interval of 45.6-49.6 (95% confidence level). This result shows good precision. The results on the I.E.S. are consistent with the conclusions on the appraisal of traumatic experiences. The reported high numbers of traumatic experiences may explain the high scores on the I.E.S. However, this conclusion has to be read with care. The I.E.S. is not validated in Sierra Leone and may therefore be subject to differences in understanding some questions. Moreover the cut-off scores may prove to be quite different then the ones used by us. Despite these considerations, high levels of traumatic stress are evident, since even when the cut of score is raised to 55 (more then doubled), 63 people (25%) still suffer from severe traumatic stress or even PTSD. 4. Physical health (Section 4) 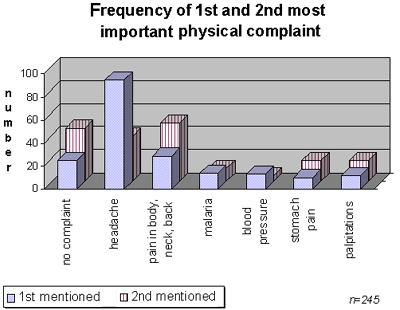
People suffering from traumatic stress and PTSD often have physical complaints like headache, stomach problems, body pain, dizziness or palpitations. Frequently the complaints cannot be related to a physical disease or disorder. Nevertheless, the physical complaints are expressed in frequent visits to the overburdened health care settings. People continue to search for a physical cure to alleviate their emotional problems. Medical people are not aware of or feel powerless against the somatizing patient and offer medication. Despite the costs both to the patient and the health system, this situation is frequently found in health settings in violent contexts. Some indicators of physical health and medical needs are described below. Since the onset of the violence, the majority of the respondents (85%) perceived their health to be worse than before. Consistent with this finding is the occurrence of unclear physical symptoms reported by the majority of the respondents (78%). As a result, 42% of the respondents visited the health post or clinic at least twice in the four weeks prior to the survey.
The table above is an overview of perceived health, the occurrence of unclear symptoms and the number of health post/clinic visits (Rarely = 1; Sometimes= 2.3; Often= 4+). The results of the fourth section (physical health) confirm the tendencies reported earlier. Traumatic stress associated with physical complaints (like headache (39%) and body pains (12%)) is reported most frequently. The visits to health facilities are relatively high (42%). The majority takes medication (e.g. paracetamol, panadol, vitamins, chloroquine). V. Conclusions The survey among respondents from all suburbs of Freetown indicates high levels of traumatic stress among the population surveyed. Every indicator (experienced events, Impact of Event Scale and Physical Health) points in the same direction. The indicators are discussed below. The responses on the second section appraise the traumatic experiences of the respondents. The high percentages of certain events (starvation (99%), witnessing wounded people (90%), having lost someone close (at least 50%)) result in a clear conclusion that most respondents living in all parts of Freetown have experienced at least one traumatic experience. It is likely they have been subjected to many more. The Impact of Event Scale (Horowitz, Wilner & Alvarez, 1979) indicates high levels of traumatic stress and PTSD in the survey population (99%). The final score on the I.E.S. is constructed around two clusters of reactions: intrusions (e.g. flashbacks, reliving of events) and avoidance (e.g. evasion of situations, amnesia). Neither of them contributed significantly more to the overall PTSD score. The outcome of the Impact of Event Scale (I.E.S.) is not conclusive and should be considered with care since the I.E.S. questionnaire is not validated for Sierra Leone and the cut-off scores applied in this report are based on Western European data. The outcomes on the I.E.S. should not lead to the conclusion that almost everybody in Sierra Leone is traumatized and suffers from PTSD or other mental health problems. However, the high scores on the I.E.S. are supported by the outcomes on the appraisal of traumatic experiences (second section). The results of the last section (physical health) confirm the tendencies reported earlier. Traumatic stress associated with physical complaints (like headache (39%) and body pains (12%)) is reported most frequently. The visits to health facilities are relatively high (42%). The high levels of traumatic stress or even PTSD indicate a clear need for psychosocial or mental health interventions to address the needs of the survivors of violence in Freetown. To focus humanitarian aid only on material restoration and physical needs denies the shattered emotional worlds of the population, and ignores the ruined basic assumptions of trust and the benevolence of human beings. It leaves unaddressed the broken morale of the survivors and the spiritual consequences of war. A population that is in general psychologically healthy can prosper and overcome the burdens of the past. Psychologically healthy people can also solve their disagreements in less violent ways. Helping traumatized people is a matter of restoring the bond between the individual and the surrounding system of family, friends, community and society. To overcome mass traumatization as in the case of Sierra Leone, the healing capacity of family and community systems must support people in their coping with extreme stress and more severe mental health problems. Psychosocial and mental health programs are evident tools in this process and should not be overlooked. The involvement of Sierra Leoneans in these programs is of crucial importance. Annexes
Table 1: Key areas and cluster distribution
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
© 2005 Doctors Without Borders/Médecins Sans Frontières (MSF)
|

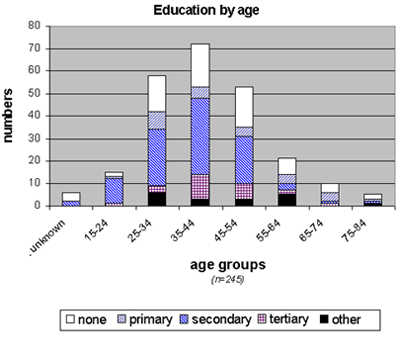 The majority has attended primary school, also in the older age groups;
on average 30% have not had formal education.
The majority has attended primary school, also in the older age groups;
on average 30% have not had formal education.